Anorexia (pronounced an-uh-rek-see-uh)
(1) In clinical medicine, loss of appetite and inability to eat.
(2) In psychiatry, as anorexia nervosa, a defined eating disorder characterized by fear of becoming fat and refusal of food, leading to debility and even death.
(3) A widely-used (though clinically incorrect) short name for anorexia nervosa.
1590–1600: From the New Latin, from the Ancient Greek ἀνορεξία (anorexía), the construct being ἀν (an) (without) + ὄρεξις (órexis) (appetite; desire). In both the Greek and Latin, it translated literally as "a nervous loss of appetite". Órexis (appetite, desire) is from oregein (to desire, stretch out) and was cognate with the Latin regere (to keep straight, guide, rule). Although adopted as a metaphorical device to describe even inanimate objects, anorexia is most often (wrongly) used as verbal shorthand for the clinical condition anorexia nervosa. The former is the relatively rare condition in which appetite is lost for no apparent reason; the latter the more common eating disorder related to most cases to body image. Interestingly, within the English-speaking world, there are no variant pronunciations. Anorexia & anorexiant are nouns, anorexic is a noun & adjective and anorexically is an adverb; the noun plural is anorexics
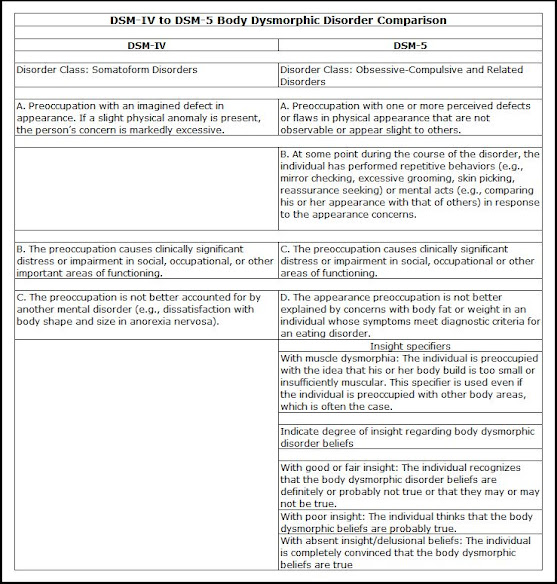
Anorexia Nervosa and the DSM
A classic pro-ana image.
The pro-ana community has created its own sub-set of standard photographic angles, rather as used car sites typically feature certain images such as the interior, the odometer, the engine etc. Among the most popular images posted on "thinspiration" pages are those which show bone definition through skin and, reflecting the superior contrast possible, there's a tendency use grayscale, usually converted from color originals. The favored body parts include the spine, hip bones, clavicles (collar bones) and the shoulder blades. Although documented since antiquity, the condition in its modern form wasn't noted in western medical literature until an 1873 paper presented to the Royal College of Physicians (RCP) called “Anorexia Hysterica”, a description of a loss of appetite without an apparent gastric cause. That same year, a similar condition was mentioned in a French publication, also called “l’anorexie hystérique”, and described food refusal combined with hyperactivity. Although the author of the earlier work had within a year changed the descriptor to “Anorexia Nervosa”, the implication in all these papers was of an affliction exclusively female, something very much implied in “l’anorexie hystérique”, hysteria then a mainstream diagnosis and one thought inherently "a condition of women".
After its acceptance as a psychogenic disorder in the late nineteenth century, anorexia nervosa (AN) was the first eating disorder placed in the American Psychiatric Association's (APA) Diagnostic and Statistical Manual of Mental Disorders (DSM). In the first edition (DSM-I (1952)), it was considered a psycho-physiological reaction (a neurotic illness). In the DSM-II (1968), it was listed with special symptoms & feeding disturbances, which also included pica and rumination. In DSM-III (1980), eating disorders were classified under disorders of childhood or adolescence, perhaps, at least in part, contributing to the under-diagnosis of later-onset cases. At that time, the American Psychiatric Association (APA) created two specific categories that formally recognized the diagnosis of eating disorders: AN and binge eating (called bulimia in DSM-III and bulimia nervosa (BN; the obsessive regurgitation of food) in both the revised DSM-III (1987) and DSM-IV (1994). In the DSM-IV, all other clinically significant eating disorder symptoms were absorbed by the residual categories of eating disorder not otherwise specified (EDNOS) and binge-eating disorder (BED), noting the disorders were the subjects for further research. Subsequently, When the DSM-IV was revised (2000), eating disorders moved to an independent section. The DSM-5 (2013) chapter for eating disorders added to the alphabet soup. In addition to pica, AN, BN and BED, DSM-5 added avoidant/restrictive food intake disorder (ARFID) and other specified feeding or eating disorder (OSFED), the latter including some other peculiar pathological eating patterns, like atypical AN (where all other criteria for AN are met, but weight is in the normal range).
Strikingly,
although there are Western countries in which anorexia kills more people than
road trauma, even within among mental health clinicians there appears to be
some reticence in dealing with patients.
Despite it being a mental health condition with a high fatality rate,
there seems still a perception the root cause is “mere vanity” and something of
a self-indulgent among young, white, middle class females who spend too much
time on TikTok and Instagram middle; essentially, they’re often thought
exemplars of the “worried well”. The
problem is acknowledged by some specialists who claim because of these perceptions
within the mental health community; treatment regimes have in recent decades
shown few advances. Among psychiatrists
and psychologists the notion of anorexia being a “self-inflicted problem of the
privileged” is not universal but critics do say that despite the disturbing
death toll (some studies claiming a fifth of patients die within 20 years),
there is still some tendency to trivialise the condition. In Australia, the Butterfly Foundation is a national
charity offering services to those affected by eating disorders and body image
issues, the coverage not limited to sufferers but available also to friends,
families and support communities. Although
Anorexia Nervosa is the best known of the eating conditions, Butterfly Foundation
functions as a kind of clearing house for all, listing the most frequently diagnosed
as:
Anorexia
Nervosa is characterised by restrictive eating that leads to a person being
unable to maintain what is considered to be a normal and healthy weight. People
experiencing Anorexia Nervosa possess an intense fear of gaining weight or
becoming overweight, no matter their current weight and appearance.
Bulimia
Nervosa is characterised by repeated episodes of binge eating, followed by
compensatory behaviours, such a purging or excessive exercise. People
experiencing Bulimia Nervosa often place an excessive emphasis on their body
shape or weight.
Binge
Eating Disorder is characterised by episodes of eating large amounts of food
over very short periods of time, with no compensatory behaviours. People who
experience binge eating often feel a loss of control during episodes of binge
eating.
Unspecified
Feeding or Eating Disorder (UFED) refers to disordered feeding or eating
behaviour that causes clinically significant distress but which does not meet
the full criteria for any of the other eating disorder categories. UFED is one
of the most common eating disorders.
Other Specified Feeding and Eating Disorders (OSFED) may
present with many symptoms of other eating disorders, but where the person
doesn’t meet the full criteria for diagnosis of those eating disorders. OSFED
is no less serious and with treatment, recovery is possible.
Disordered
eating is a disturbed and unhealthy eating patterns. They can include
restrictive dieting, compulsive eating or skipping meals. Disordered eating
behaviours, and in particular dieting are the most common indicators of the
development of an eating disorder.
Avoidant/Restrictive
Food Intake Disorder (ARFID) involves significant aversion and avoidance of
food and eating, and may include highly selective eating habits, disturbed
feeding patterns, or both.
PICA is an
eating disorder where people eat things that aren’t considered food. For
example, they may eat dirt, chalk, soap, hair, laundry detergent, among other
things.
Orthorexia isn’t currently recognised as an official eating disorder diagnosis, however there is growing recognition that this may be a distinct eating disorder. It involves an obsession with healthy, or “clean” eating. People will often obsess about the benefits of healthy foods, food quality, but not necessarily quantity of food.